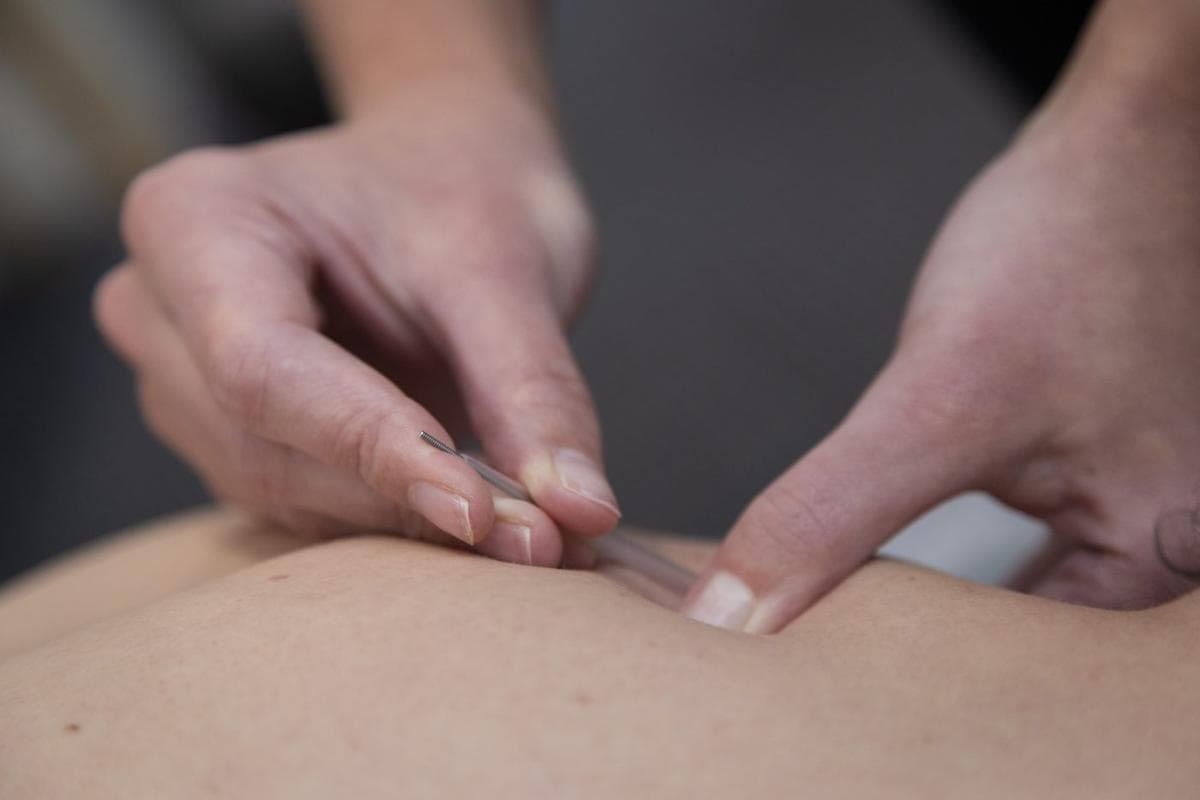
Dry needling divides people. Some patients swear by it. Others think it's expensive theatre — a placebo dressed up in clinical clothing. The honest answer, backed by the evidence, sits somewhere more specific than either camp tends to admit.
Here is what dry needling actually does, where the evidence supports it, where it falls short, and exactly how we use it at Move.
What dry needling actually is
Dry needling involves inserting a thin filiform needle — identical to an acupuncture needle — directly into a myofascial trigger point: a hyperirritable spot within a taut band of skeletal muscle that produces local tenderness and often a referred pain pattern when compressed or needled.1
The needle contains no medication — hence "dry." The mechanism is mechanical, not pharmacological. When the needle penetrates the trigger point, it provokes a local twitch response — an involuntary contraction of the taut muscle fibres — which is associated with a release of tension in that band and a reduction in the nociceptive (pain-signalling) activity in the area.5
It is important to distinguish dry needling from acupuncture. Acupuncture is a traditional Chinese medicine practice based on meridians and energy flow. Dry needling is a western, anatomically-based intervention targeting specific neuromuscular structures. They use the same needle — the theoretical framework is completely different.
What the evidence actually shows
The evidence base for dry needling is legitimate — but it is more specific than most clinicians or patients realise. The strongest evidence is for short-term pain reduction and improved pressure pain threshold in myofascial trigger point conditions, particularly in the upper quarter: neck, shoulder, and upper back pain.2,7
A 2017 systematic review and meta-analysis of 12 randomised controlled trials found that dry needling by physiotherapists was effective for reducing pain and improving function in musculoskeletal conditions — with moderate-to-large effect sizes at short-term follow-up compared to control interventions.4 A 2013 meta-analysis specific to upper quarter myofascial pain found significant improvements in pain intensity immediately post-treatment and at four weeks compared to sham needling.7
Where the evidence is strongest
- Neck and shoulder myofascial pain — the most consistent evidence base
- Upper back trigger points, including trapezius and levator scapulae
- Short-term pain relief and improved range of motion
- Reducing local muscle tension and pressure pain threshold
- As an adjunct to active rehabilitation — not as a standalone treatment
Where the evidence is weaker
- Long-term outcomes — effects at 3–6 months are less consistent across studies
- Structural injuries (tendons, joints, ligaments) — dry needling does not repair these
- Lower limb conditions — evidence base is smaller and less robust than upper quarter
- As a standalone treatment for complex or loading-related injuries
Why it works — the physiology
When a needle penetrates a trigger point and elicits a local twitch response, several things happen at a tissue level. The involuntary contraction followed by relaxation of the taut muscle fibres disrupts the dysfunctional motor endplate activity that perpetuates the trigger point. Local circulation improves — trigger points are associated with low oxygen tension and high concentrations of inflammatory mediators, and the needling response helps to flush and normalise the local chemical environment.5
At a central level, needling stimulates the release of endogenous opioids and activates descending pain inhibition pathways — similar to other forms of manual therapy and exercise. This is partly why the effect isn't purely local and why some patients report broader pain relief beyond the specific area treated.6
The net effect is a meaningful reduction in local muscle tension, improved range of motion, and a window of reduced pain sensitivity. That window is the clinical opportunity — and what you do with it determines whether the treatment is worthwhile or not.